Overemployed Health Insurance: Dual Coverage Guide 2026
December 22, 2023 | by overemployedtoolkit.com

Overemployed Health Insurance: Dual Coverage Guide 2026
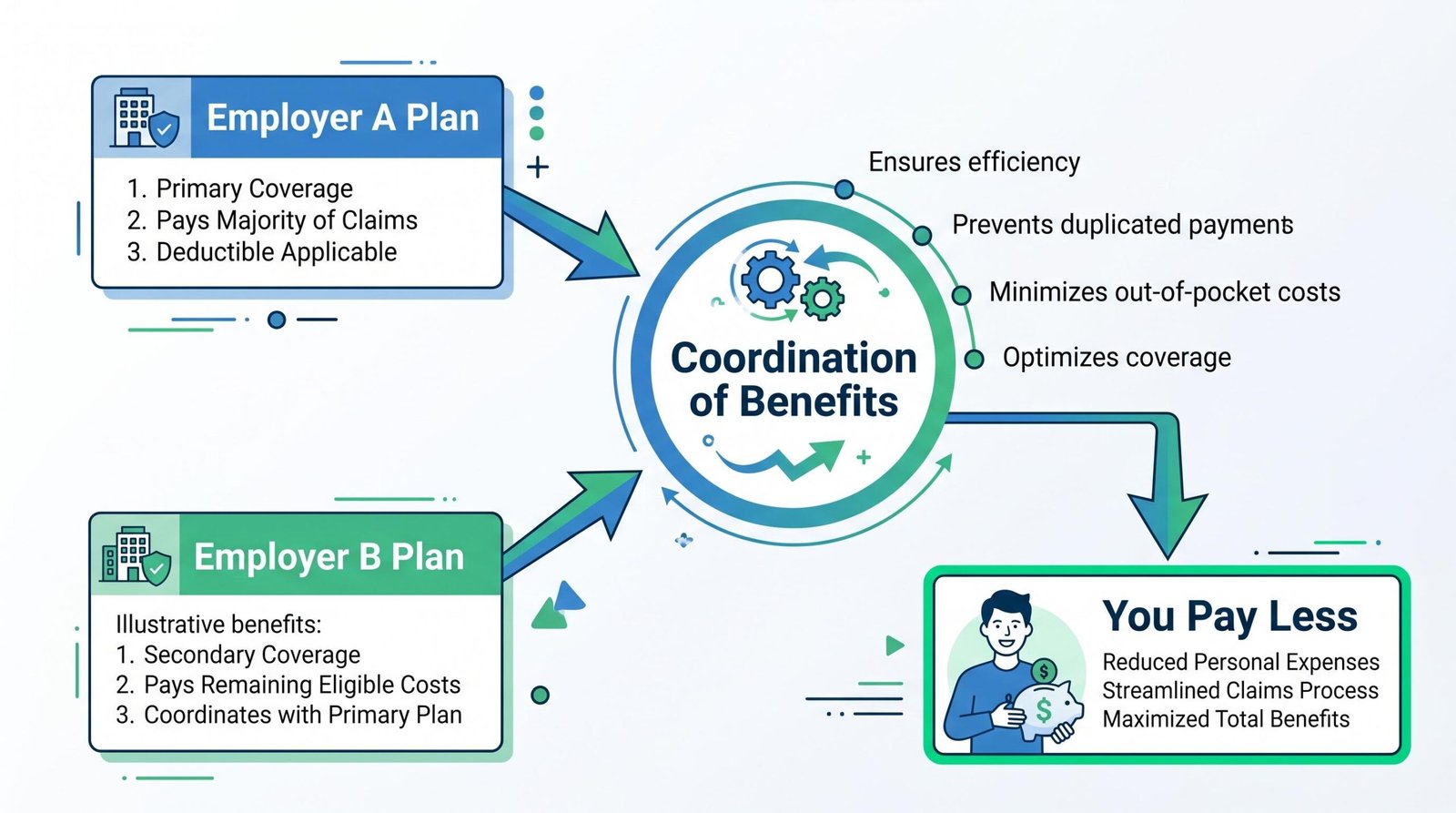
Overemployed health insurance works through coordination of benefits: one employer plan acts as primary and pays claims first, the other acts as secondary and may cover some remaining costs. Federal law allows dual enrollment, but the HSA contribution rules under IRC section 223 disqualify anyone covered by a non-HDHP plan, which traps most multi-job workers.

If you are working multiple remote jobs, your benefits enrollment paperwork suddenly becomes a strategic decision rather than a checkbox. Two employers means two health plan offers, two open-enrollment windows, and a maze of rules that can either save you thousands or quietly disqualify you from a triple-tax-advantaged HSA. This guide walks through every layer of the decision the way an OE worker actually faces it.
Can You Have Health Insurance from Two Jobs at Once?
Yes. Federal law does not bar you from enrolling in two employer-sponsored health plans at the same time, and insurers process millions of dual-coverage claims every year through coordination of benefits (COB). Healthcare.gov confirms that dual coverage through two employers, a spouse plus your own employer, or a parent plus an employer (if under 26) is fully legal and routine.
What does sometimes raise flags is enrolling yourself as the primary subscriber on two plans at once. Insurers running COB checks may notice the duplicate primary enrollment and ask questions, which is one of the ways HR departments occasionally detect workers holding two full-time jobs. Most OE workers manage this risk by enrolling in only one plan as primary and either declining J2 coverage or accepting it as a deliberate secondary layer.
Two practical reasons OE workers double-enroll anyway:
- Bridge protection during onboarding. Your J1 coverage may already be active when J2 enrollment opens. Carrying both for one or two months prevents a gap if either job ends unexpectedly.
- Filling specific coverage gaps. If J1 has a strong PPO network but weak dental, and J2 has excellent dental but a narrower medical network, dual coverage can stack benefits where they complement each other.
How Coordination of Benefits Works
Coordination of benefits is the industry rulebook insurers use to decide which plan pays first when you have two. It was developed by the National Association of Insurance Commissioners and is followed by most fully insured plans, though self-insured ERISA plans can deviate. The default rule for an OE worker enrolled in two of their own employer plans: the plan with the earlier effective date on your coverage usually pays first, unless one plan lacks a COB provision (in which case that plan is automatically primary).
The secondary plan does not always pay everything left over. Three formulas dominate, and the difference can be hundreds of dollars per claim, as LegalClarity explains in its NAIC summary:
| Primary Plan | Secondary Plan | What Gets Covered | Out-of-Pocket Impact |
|---|---|---|---|
| J1 PPO pays per its terms first | J2 PPO using Traditional COB | Secondary pays the difference between what primary paid and the secondary plan’s normal benefit, up to 100% of allowed charges | Often $0 after both plans process; best outcome for the patient |
| J1 PPO pays per its terms first | J2 PPO using Maintenance of Benefits | Secondary pays only what it would have paid as primary, minus what J1 already paid | You may still owe deductible or coinsurance amounts |
| J1 PPO pays per its terms first | J2 PPO using Non-Duplication | Secondary pays only the difference between its benefit and the primary’s payment – if primary paid more, secondary pays nothing | Often $0 from secondary; you pay the gap yourself |
| Your employer plan | COBRA from a previous job | Active employer plan is primary, COBRA is secondary per NAIC rules | Same as Traditional or MOB depending on the COBRA plan’s formula |
ValuePenguin notes a critical limitation: most secondary plans will not pay your primary’s deductible, copay, or coinsurance unless they use Traditional COB. Check both plan documents for the specific COB method before assuming two plans equals zero out of pocket.
The HSA Trap – Why Being on Two Plans Can Cost You
This is the single biggest mistake the OE community makes. The Health Savings Account is the most powerful tax-advantaged account in the U.S. code: pre-tax contributions, tax-free growth, and tax-free withdrawals for medical expenses. To contribute, you must be covered by an HSA-qualified High Deductible Health Plan (HDHP) and have no other disqualifying coverage.
IRS Publication 969 states the rule plainly: to be HSA-eligible, “you have no other health coverage except what is permitted under Other health coverage.” If your J1 enrolls you in an HDHP and J2 enrolls you in a PPO, even if the PPO is a low-value plan you never use, you lose HSA eligibility for every month you have that PPO coverage. The Congressional Research Service confirms that individuals are disqualified “if they also are covered under a spouse’s policy for the same benefits and that spouse’s policy is not an HSA-qualified HDHP” – the same logic applies to a second employer’s policy.
The permitted exceptions are narrow: workers’ compensation, specific-disease coverage, fixed indemnity hospital plans, dental, vision, and long-term care. A standard PPO from J2 is not on that list. IRS Revenue Ruling 2004-38 even disqualifies someone whose only “second coverage” is a prescription drug rider that pays before the HDHP deductible is met.
The 2026 contribution limits, per the IRS, are $4,400 for self-only HDHP coverage and $8,750 for family HDHP coverage. Catch-up contributions of $1,000 are available at age 55. For an OE worker in the 32% federal bracket plus state tax, losing HSA eligibility for a year can mean roughly $1,500 to $3,000 in lost tax savings.
Three practical paths if you want to keep your HSA:
- Decline J2 medical coverage entirely. Take J2’s dental, vision, and life benefits if useful – those do not disqualify HSA contributions – but skip the medical plan.
- Match HDHP to HDHP. If both employers offer HDHP options, you can technically dual-enroll without losing HSA eligibility, though COB still applies and you waste premium dollars on overlapping coverage.
- Stop HSA contributions for the months of overlap only. HSA eligibility is determined month by month, so even a partial year of HSA contributions has value. Pro-rate carefully and avoid the last-month rule trap that requires you to maintain HDHP coverage through the following year’s testing period.
Choosing Which Employer’s Plan to Use as Primary
Picking the right primary plan is the single highest-leverage decision in your benefits stack. The plan you choose determines your network, your deductible, your in-network specialists, and whether you keep HSA eligibility. Run the comparison on five variables before open enrollment closes:
- Total annual cost. Premium plus expected out-of-pocket. Use last year’s claims as a baseline. For most healthy OE workers, an HDHP with HSA beats a PPO when you factor in the tax savings on contributions.
- Network strength in your zip code. A cheaper plan with no in-network specialists near you is not cheaper. Check that your current physicians and your nearest hospital system are in-network.
- Employer contribution. Some employers contribute $500 to $2,000 directly to your HSA. Free money should rarely be left on the table.
- Out-of-pocket maximum. This is the worst-case number that matters during a serious medical event. The 2025 federal cap for HDHPs sits at $8,050 self-only and $16,100 family per the IRS.
- Stability of the employer. Tying your primary to the more secure job reduces the chance of a mid-year scramble. If J1 is the long-tenure cash cow and J2 is the newer or riskier role, keep primary on J1.
For most overemployed workers, the cleanest play is: pick one HDHP from your most stable employer as primary, fund the HSA up to the limit, and decline medical coverage at the second job. Take the cash equivalent if your employer offers an opt-out credit.
The COBRA Bridge Strategy
Job transitions are when OE workers most often need a bridge. The Consolidated Omnibus Budget Reconciliation Act lets you continue your former employer’s group health plan after a qualifying event – typically termination (other than gross misconduct) or a reduction in hours. The U.S. Department of Labor confirms COBRA coverage generally lasts 18 months, extends to 29 months for SSA-determined disability, and can stretch to 36 months for spouses and dependents after certain second qualifying events.
The cost is the catch. Under the DOL’s COBRA guide, you pay up to 102% of the full premium (the employee plus employer share plus a 2% administrative fee). Disability extension premiums can rise to 150% of plan cost. For a typical family plan that costs an employer $1,800 per month, your COBRA premium runs roughly $1,836 monthly.
Where COBRA earns its keep for an OE worker:
- You quit J1 and J2 is still onboarding. COBRA from J1 covers you for the 30 to 90 day gap before J2 benefits begin. You have 60 days from your loss-of-coverage date to elect, and coverage applies retroactively.
- You are losing both jobs and need to ride out an open enrollment window. COBRA preserves your existing doctor relationships and prescription formularies while you shop the ACA marketplace.
- You are mid-treatment with a specific specialist or in-network hospital. Switching plans mid-course can break a treatment plan. COBRA keeps the same network and the same accumulated deductible for the rest of the calendar year.
If you take a new job with health benefits before exhausting COBRA, the new employer plan becomes primary and COBRA acts as secondary per NAIC rules. Most workers drop COBRA at that point because paying full premium for a secondary is rarely worth it.
Tax Implications of Multiple Employer Health Insurance
Employer-paid health insurance premiums are tax-free under Section 106 of the Internal Revenue Code, and the employee share you pay through payroll deduction comes out pre-tax under a Section 125 cafeteria plan. That tax exclusion applies to both employers independently. When you carry coverage at J1 and J2 and both run premiums through cafeteria plans, you get the pre-tax treatment twice.
A few wrinkles OE workers should track:
- Healthcare FSA limits aggregate across employers. The 2026 healthcare FSA cap, per recent IRS guidance reported by financial planners covering the OE space, is $3,400 total across all employers. Contributing the full amount through both employers triggers an excess contribution that you must remove or report.
- HSA contributions also aggregate. If both J1 and J2 offer HSAs and contribute, your combined contributions plus any employer matches cannot exceed the statutory limit ($4,400 self-only or $8,750 family in 2026). Excess contributions face a 6% excise tax annually until corrected.
- W-2 Box 12 Code DD. Both employers report the total cost of your employer-sponsored coverage on Box 12 with code DD. This is informational only and not taxable, but it makes dual enrollment visible on your return.
- Premium tax credits are unavailable if either employer offers affordable minimum-value coverage per HealthCare.gov rules.
None of these create direct tax liability the way a 401(k) over-contribution does, but FSA and HSA excess contributions require active correction. We suggest tracking both employer contributions in a simple spreadsheet and adjusting your year-end elections before December to stay under the combined cap.
When the ACA Marketplace Makes More Sense
Most OE workers earn too much to qualify for ACA premium tax credits, so the marketplace appears irrelevant. There are still three scenarios where HealthCare.gov beats employer coverage.
One. Your employer coverage fails the affordability test. Under HealthCare.gov rules, if your share of the lowest-cost employee-only premium exceeds 9.12% of household income (the 2023 threshold, indexed annually), your employer plan is considered unaffordable and you may qualify for marketplace subsidies even with an offer of coverage.
Two. You want network flexibility that no employer plan offers. Marketplace plans sometimes include broader PPO networks than the narrow HMO-style plans common at large employers, especially if you live in a different state than your employers.
Three. You are between jobs and need a longer bridge than COBRA’s price tag justifies. A Silver or Bronze marketplace plan often costs less than COBRA’s 102% premium, and losing employer coverage triggers a 60-day Special Enrollment Period on HealthCare.gov. We suggest running both quotes side by side before defaulting to COBRA.
Before electing to drop both employer plans for the marketplace, confirm that doing so does not violate your offer letters. Overemployment legality generally turns on contractual exclusivity clauses, not benefits choices, but reading the fine print never hurts.
Frequently Asked Questions
Can I be on two employer health plans at once?
Yes. Federal law does not prohibit dual enrollment. Both insurers apply coordination of benefits rules to decide which plan pays first. Some self-insured ERISA plans have anti-duplication clauses, so read the plan documents.
Will dual coverage cover 100% of my medical bills?
Only if both plans use Traditional COB. Plans using Maintenance of Benefits or Non-Duplication formulas often leave you on the hook for deductibles and coinsurance even with two plans active.
Can I contribute to an HSA if I have two health plans?
Only if every plan covering you is an HSA-qualified HDHP and you have no other disqualifying coverage. A standard PPO at J2 disqualifies you from HSA contributions under IRC section 223, per IRS Publication 969.
How long can I stay on COBRA between jobs?
Generally 18 months after termination or hours reduction. The Social Security Administration disability extension can stretch it to 29 months, and second qualifying events can extend coverage to 36 months for spouses and dependents.
Should I take the ACA marketplace instead of my employer plan?
Usually no, because OE income disqualifies most workers from subsidies. The marketplace wins when your employer coverage fails the 9.12% affordability test, when you need a broader network, or when you need a cheaper bridge than COBRA’s 102% premium between jobs.
Will my second employer find out I am dual-enrolled?
Possibly. Insurers running COB checks may notify the secondary plan administrator, and benefits departments sometimes review these flags. Enrolling as primary on only one plan and declining medical at the other avoids the issue entirely.
What happens to my HSA if I become ineligible to contribute?
You keep the account and every dollar in it. The funds continue to grow tax-free and can be spent on qualified medical expenses without penalty. You simply cannot make new contributions for months you are ineligible.
RELATED POSTS
View all